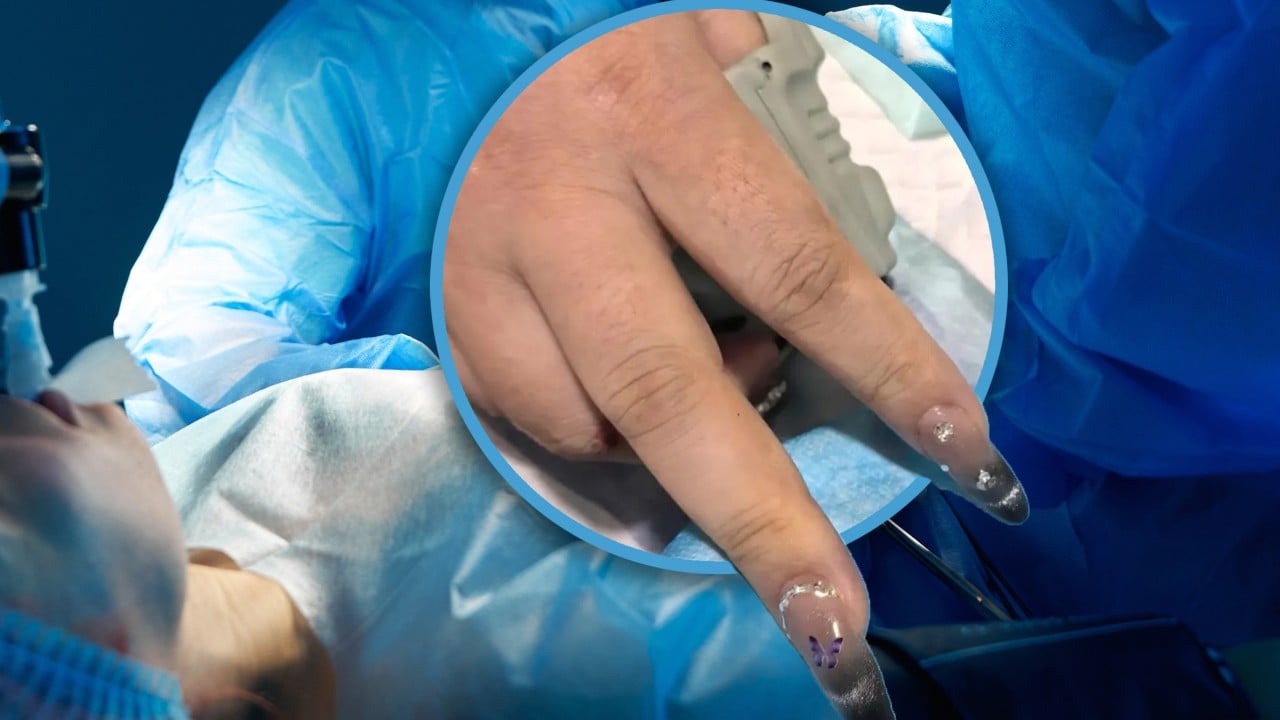
When a woman arrived at an emergency room in China with a life-threatening condition, doctors faced a barrier they weren't trained to cut through with a scalpel. Her long, reinforced acrylic nails made it impossible to monitor her blood oxygen levels, a critical data point during surgical anesthesia. Standard hospital equipment—specifically the pulse oximeter—cannot "see" through the dense pigments and chemical layers of modern nail enhancements. In a desperate move that highlights a growing gap between cosmetic trends and emergency medicine, the hospital had to summon a professional manicurist to the operating theater to grind away the plastic before the medical team could proceed.
This isn't just a quirky viral story from a provincial hospital. It is a loud warning for a global healthcare system currently unprepared for the "unremovable" nature of modern beauty standards.
The Science of the Blind Pulse Oximeter
To understand why a few grams of acrylic can derail an entire surgical team, you have to look at how we measure life. The pulse oximeter is a ubiquitous clip placed on a patient's fingertip. It works by emitting two wavelengths of light—red and infrared—through the nail bed and the tissue of the finger. By measuring how much light is absorbed by the blood, the device calculates the oxygen saturation ($SpO_2$).
When a patient is under anesthesia, their ability to breathe is managed by machines. If oxygen levels drop, the oximeter is the first line of defense. It is the "canary in the coal mine."
However, modern gel polishes and acrylics are engineered for durability. They contain polymers and pigments like titanium dioxide or metallic glitters that effectively block or scatter these light waves. Darker colors such as navy, black, or deep red are particularly notorious for causing false readings or total device failure. When the sensor fails, the anesthesiologist is left flying blind. They are forced to rely on more invasive methods, such as arterial blood gas draws, which involve needles and valuable minutes that a patient in shock simply does not have.
The Myth of the Easy Removal
The medical community often assumes that anything on a patient’s body can be removed in an emergency. Clothes are sheared off with trauma shears. Rings are cut with specialized saws. But nail enhancements are a different beast entirely.
Unlike traditional nail polish, which dissolves with a quick swipe of acetone, "soak-off" gels require twenty minutes of chemical immersion. Hard gels and acrylics often require electric files (e-files) and high-grit abrasives to thin the material.
Most emergency rooms are stocked with gauze, sutures, and defibrillators. They do not carry high-speed rotary tools or specialized carbide drill bits. This creates a dangerous friction point where medical professionals must choose between delaying care to find a way to strip the nail or proceeding with a significant blind spot in patient monitoring. In the case of the Chinese hospital, the decision to call a manicurist was a pragmatic, if unorthodox, solution to a lack of institutional tools.
Why Hospital Policy Hasnt Caught Up
We are seeing a massive surge in the popularity of long-wear nail tech. The global nail care market is a multi-billion dollar industry, yet hospital intake protocols remain stuck in the 1990s. While elective surgery centers often provide "pre-op" instructions telling patients to remove polish, the emergency department has no such luxury.
There are three primary reasons for this systemic failure:
- Equipment Stagnation: Pulse oximeter technology has not fundamentally changed in decades. While some newer sensors claim to work through light polish, they are expensive and not yet the standard in high-volume public hospitals.
- Gendered Medical Blindness: There is a historical tendency in medicine to overlook the clinical implications of "feminized" beauty products. If men commonly wore a piece of hardware that blocked vital sign monitoring, hospitals would likely have a standard tool to remove it.
- The Rise of "Hard" Enhancements: The shift from air-dry polish to UV-cured plastics has changed the physical properties of the nail. It is no longer a coat of paint; it is a structural modification.
The Risks Beyond the Oximeter
The complications extend beyond just light absorption. In a surgical environment, the area under long or artificial nails is a haven for bacteria. Studies have repeatedly shown that subungual (under the nail) areas in patients with enhancements harbor higher concentrations of pathogens, including Pseudomonas and Staphylococcus.
In a trauma situation, where a patient might need an emergency IV or a finger-prick blood test, these enhancements complicate the process. Furthermore, if a patient requires an MRI, certain metallic pigments in high-end "cat-eye" or chrome polishes can actually heat up, potentially causing burns to the nail bed.
Redesigning the Emergency Intake
If hospitals are to avoid the theater of calling in a manicurist for a "code blue," the infrastructure must change. This involves a two-pronged approach.
Hardware Adaptation
Hospitals need to invest in "earlobe sensors" or "forehead sensors" as standard backups. These locations are less convenient than the finger but are unaffected by the $100 manicure. The problem is that these sensors are often tucked away in a drawer rather than being on the primary monitor kit.
Tactical Toolkits
Every emergency department should have a professional-grade electric nail file in its "difficult access" kit. Expecting a nurse to spend thirty minutes with a manual emery board while a patient’s lungs are failing is a failure of leadership. Training staff on how to quickly thin an acrylic nail to allow a sensor to read is now a necessary skill for the 21st-century medic.
The Responsibility of the Industry
The beauty industry also shares the burden. Manicurists are rarely taught about the medical implications of the products they apply. When a client requests a "hard gel" overlay that cannot be soaked off, there is no disclaimer about emergency medical access.
We need a shift in the "aftercare" conversation. Clients should be informed that if they are heading into a high-risk surgery or are in the late stages of pregnancy, their choice of nail enhancement could directly impact their care. It is not about vanity; it is about visibility.
A Necessary Shift in Perception
The incident in China was treated by many news outlets as a "human interest" story or a humorous anecdote about a woman's commitment to her look. This is a mistake. It was a near-miss caused by a collision between a rapidly advancing cosmetic industry and a stagnant medical equipment sector.
The next time you sit in a salon chair, or the next time a hospital administrator reviews their equipment budget, they should consider the stakes. A pulse oximeter that cannot read is just a piece of plastic. A nail that cannot be removed in sixty seconds is a medical liability.
Hospitals must stop treating this as an anomaly and start treating it as a standard complication of the modern patient. Buy the drills. Train the staff. Or find a way to see through the glitter.
Check your own nails before your next scheduled procedure; if they are dark or thick, you are your own primary safety officer. Use a clear coat or leave one finger bare. It is a small price to pay for ensuring the person holding the oxygen mask knows exactly how much you are breathing.