Geography just stopped mattering in the operating room. While most of us struggle with a laggy Zoom call, Dr. Ragheed Al-Mufti just performed a medical miracle that makes a standard video chat look like stone-age tech. This wasn't just another robotic assist. This was a 2,400-kilometer leap from London to Lisbon that actually worked.
We've heard the hype about "remote surgery" for decades. It usually involves a doctor in the next room or a few miles away. This time, the stakes were different. An Indian-origin British surgeon, working out of a console in the UK, operated on a patient in Portugal. If you think that sounds like science-fiction, you're right. It is. But it’s also the new reality of the National Health Service (NHS) and global healthcare.
The lag that didn't happen
The biggest enemy in remote procedures is latency. In the medical world, a half-second delay isn't an inconvenience. It’s a catastrophe. If a surgeon moves their hand and the robotic scalpel doesn't mirror that move instantly, the patient bleeds out.
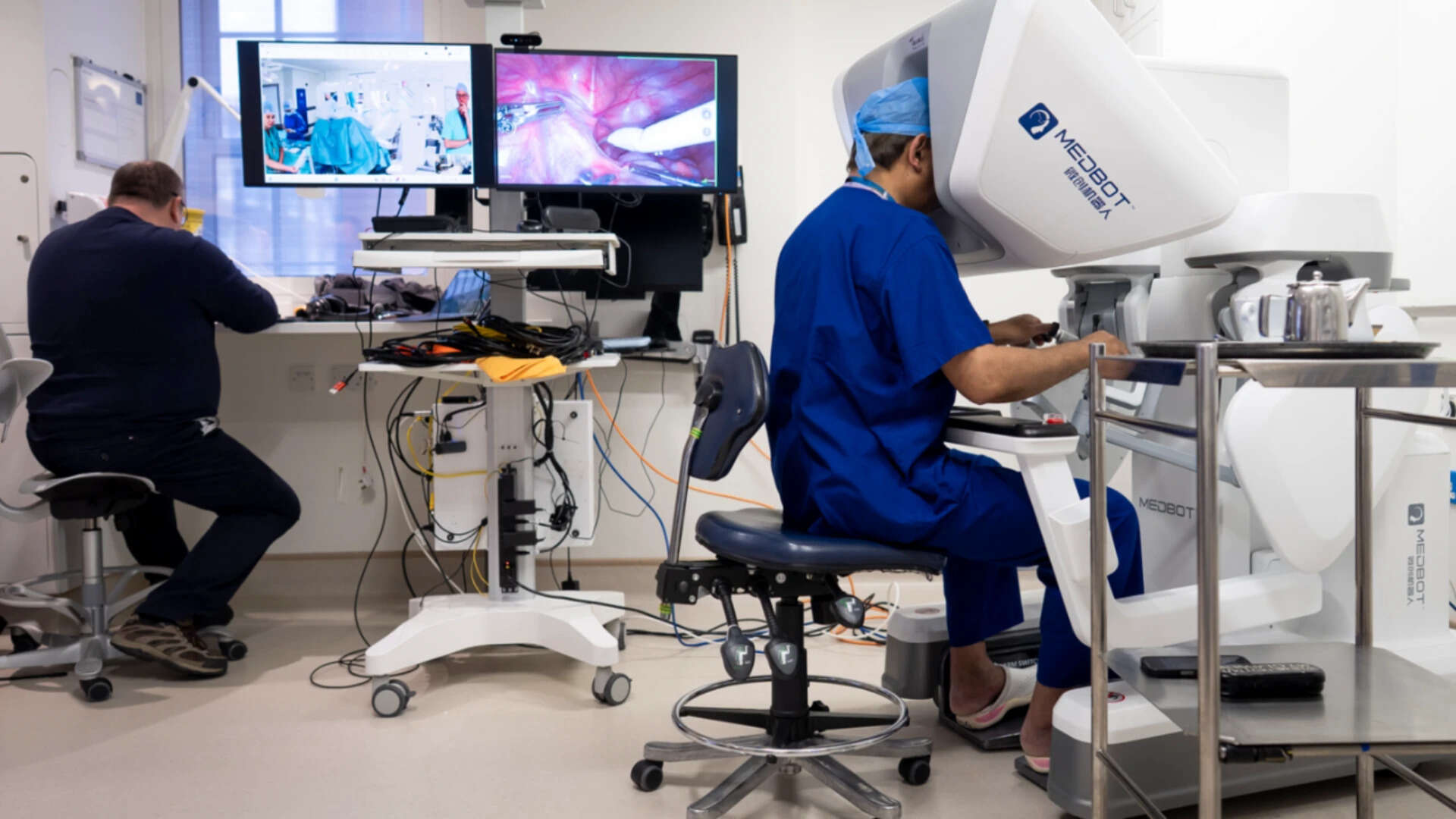
Dr. Al-Mufti, a consultant at Imperial College Healthcare NHS Trust, used a specialized high-speed fiber connection that essentially deleted the distance. The "time-of-flight" for the data was so fast the human brain couldn't perceive it. We're talking about milliseconds. He was performing a complex procedure—not a simple stitches job—using the Da Vinci system and a dedicated private network.
Most people think 5G is just for downloading movies faster. They’re wrong. This operation proved that high-bandwidth, low-latency networks are now surgical instruments. The setup allowed him to see 3D, high-definition images of the internal organs in Lisbon while sitting comfortably in London. He felt the resistance. He saw the texture. He didn't just watch; he was "there."
Why this specific surgery matters for the NHS
Let’s be honest. The NHS is under massive pressure. Long waiting lists for specialists are the norm, not the exception. Usually, if you need a world-class surgeon, you have to travel to them, or they have to fly to you. Both options are expensive, slow, and often impossible for critically ill patients.
This successful long-distance operation flips the script. It means the talent can stay in London while the "hands" work in a rural clinic or a different country entirely. We're looking at a future where your physical location doesn't dictate the quality of your healthcare. Dr. Al-Mufti’s achievement isn't just a win for his resume. It’s a proof of concept for a hub-and-spoke model of surgery that could save thousands of lives.
The precision of the robotic arms actually exceeds human capability in some ways. They don't shake. They can pivot in angles a human wrist can't achieve. When you combine that mechanical perfection with the seasoned intuition of a top-tier surgeon, the results are objectively better.
Addressing the skeptics and the technical hurdles
I know what you're thinking. What happens if the internet goes down?
It’s a valid fear. During this 2,400km procedure, there were multiple layers of redundancy. This wasn't running on a home Wi-Fi router. The team used dedicated lines with automatic failovers. If one path failed, the data rerouted in a heartbeat. Furthermore, a local surgical team was standing by in Lisbon, ready to take over manually if the connection dropped for even a second.
Safety isn't an afterthought here. It’s the foundation. The success of this operation shows that the "what-if" scenarios have been engineered into oblivion. We've moved past the experimental phase.
The human element in a digital theater
There’s a common misconception that robots are replacing doctors. That’s nonsense. The robot is a tool, much like a more advanced version of a scalpel. The brilliance of this UK-Portugal operation was Dr. Al-Mufti’s ability to interpret the digital feedback.
He's a pioneer not because he used a machine, but because he mastered the interface. His background and training at Imperial College London—one of the world's leading medical institutions—prepared him for this. It takes years to build the muscle memory required for robotic surgery. Doing it with 2,400 kilometers of cable between you and the patient requires a level of mental fortitude most can't imagine.
Transforming global health equity
Think about the implications for developing nations or remote areas. Currently, if you’re in a remote village and need specialized neurosurgery, your chances aren't great. If we can scale what Dr. Al-Mufti just did, a surgeon in London could operate on a patient in a mobile surgical unit in sub-Saharan Africa.
The hardware exists. The software is getting there. Now, the infrastructure needs to catch up. This wasn't just a "first for the UK." It was a signal to every health ministry on the planet. Invest in digital infrastructure, and you're investing in the lives of your citizens.
This event also highlights the incredible contribution of the Indian diaspora to British medicine. Dr. Al-Mufti represents a long tradition of excellence that keeps the UK at the forefront of global medical innovation.
How to prepare for the robotic shift
If you're a medical professional or even a patient, you can't ignore this. The "tele-surgeon" is a real career path now. Medical schools are already shifting their curriculum to include more simulation-based training.
For patients, the takeaway is simple. Don't be afraid of the "robot." It’s often safer than a traditional open surgery because it's less invasive. Smaller incisions mean faster recovery times and less risk of infection.
Start by asking your local healthcare provider about their robotic surgery options. Check if your insurance covers "minimally invasive" robotic procedures. If you're a student, look into biomedical engineering or specialized surgical fellowships that focus on human-machine interfaces. The era of the "local-only" doctor is ending. The era of the global specialist has arrived.
Keep an eye on the next wave of trials from Imperial College and the NHS. They’re currently looking at how to make these setups more portable. The goal is to bring the surgery to the patient, no matter where the surgeon is sleeping that night. That’s not a dream. It’s the blueprint.